Eugene Quinn for East Greenwich Schools
Why I think it's a good idea to get vaccinated
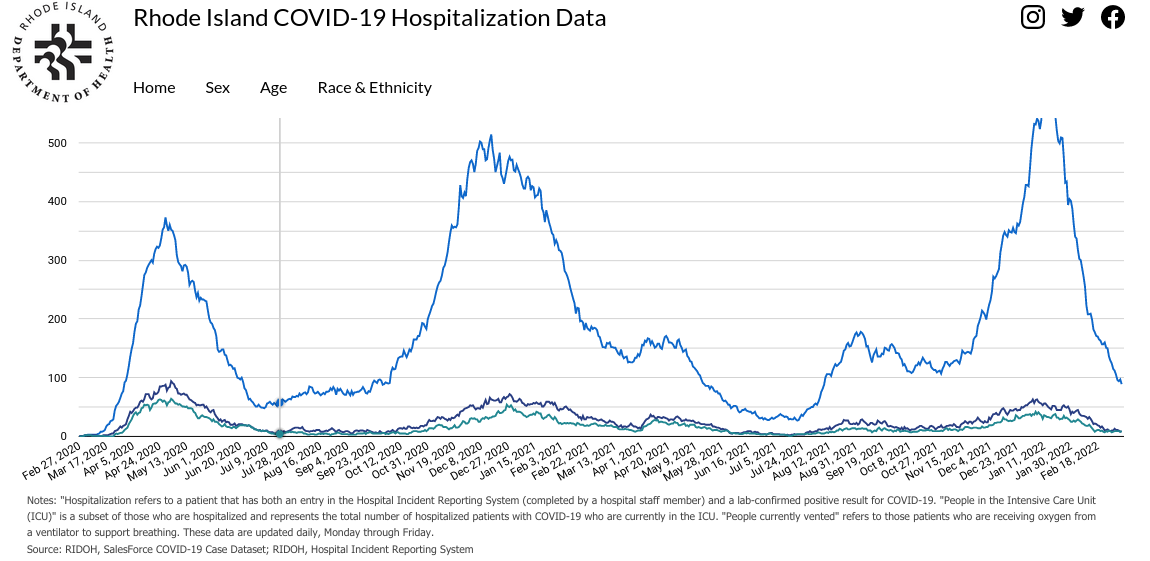
Hospital and Intensive Care Unit (ICU) capacity is closely monitored by the Rhode Island Department of Health.
The dire consequences of exceeding ICU capacity are a major concern. The dark blue graph is the number of ICU beds occupied. Heroic efforts of healthcare professionals notwithstanding, it appears that we had enough ICU beds to handle the Omicron wave in early January, 2022.Queueing Models
Queueing theory is widely used in operations research to model the capacity and operating characteristics of systems comprised of waiting lines and servers.1
One of the simplest and most widely used models is one with a Poisson arrival process, exponential service times, and a fixed number of 'servers' m.
In the Kendall notation, this is called the M/M/m model.2
This type of model gives reasonable results for a queueing system in a steady state, meaning one that has been operating long enough to converge to an equilibrium.
While it does not handle transient behavior, this type of model is useful for studying the behavior of systems under normal operating conditions.
It lends itself to 'back-of-the-envelope' models because it requires only a few parameters:

Mathematical models provide a way to evaluate 'what if' scenarios for many situations without actually having to experience and observe them.
George Box famously stated 'All models are wrong, some models are useful'. A model will never exactly reproduce the real world, but it doesn't have to as long as it is a reasonably good approximation. Real world experience with queueing models suggests that the queue length estimates they produce are within about 15% of the actual observed values, which is more than adequate for use in a quick analysis.Modeling ICU Capacity
The only parameters we need are:
Now we vary the arrival rate and observe the predicted behavior of the system.
Case 1: One arrival per day
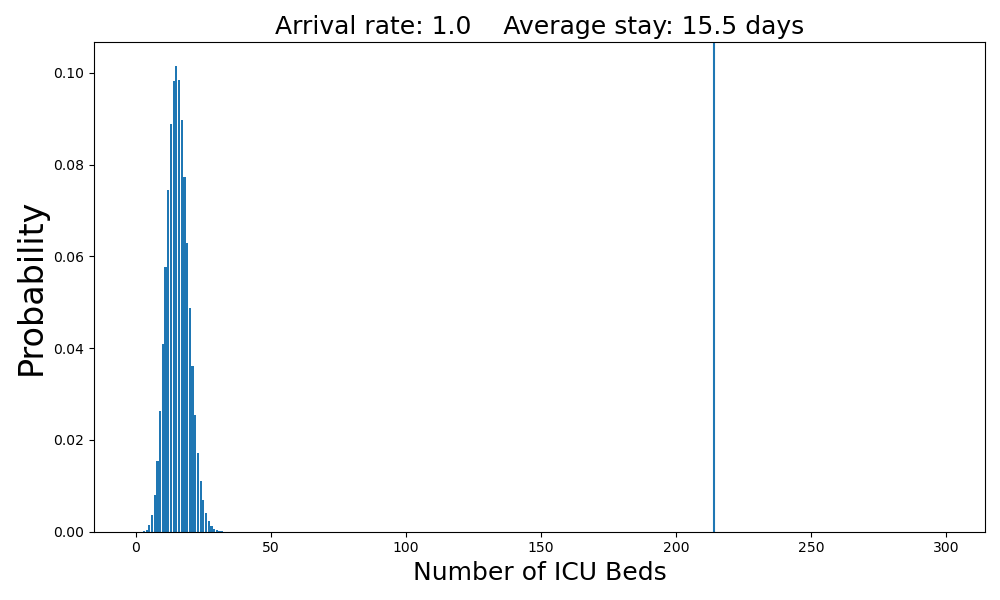
At one new ICU case per day, are well within the capacity of the system.
The average number of occupied beds is 15.5. The probability that there will not be a bed available when a patient arrives is close to zero.Case 2: Six arrivals per day
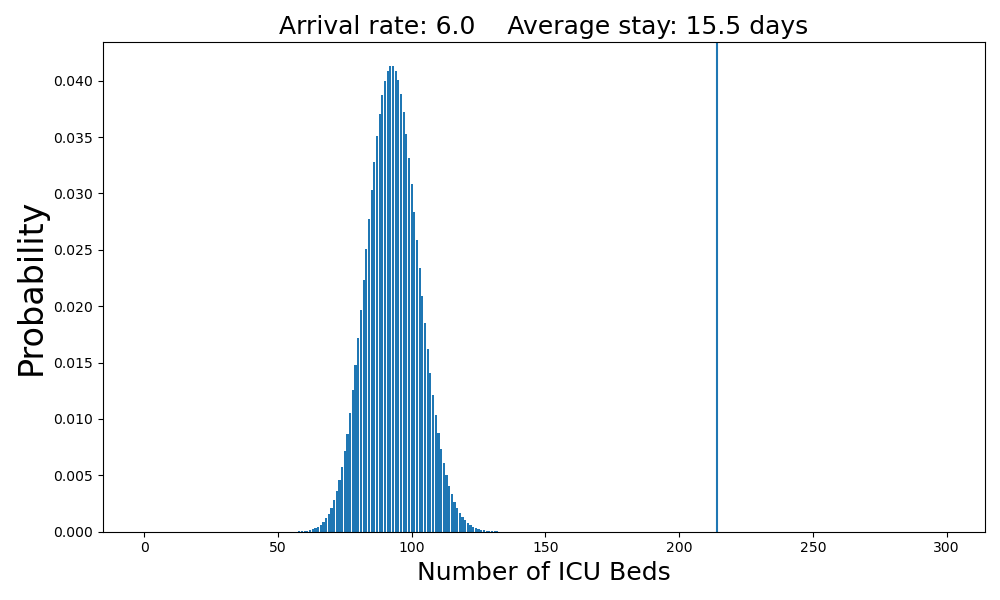
Six arrivals per day is well within the capacity of the system.
The average number of occupied beds is 93. The probability that there will not be a bed available when a patient arrives is still close to zero.Case 3: Ten arrivals per day
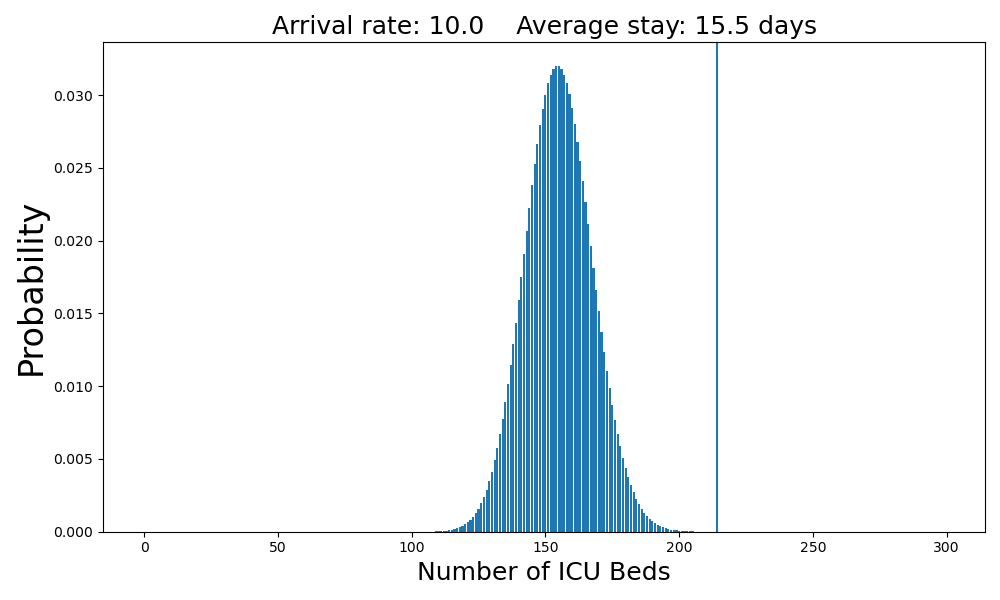
Ten arrivals per day is within the capacity of the system, but just barely.
The average number of occupied beds is 155. The probability that there will not be a bed available when a patient arrives is still close to zero.Case 4: Twelve arrivals per day
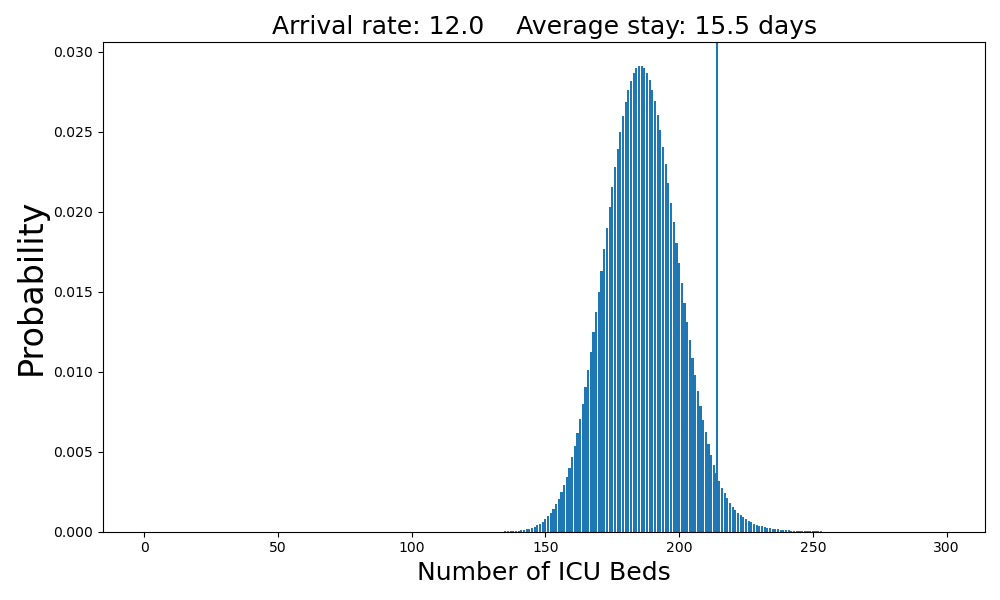
At twelve arrivals per day, the system has pretty much reached capacity.
The average number of occupied beds is 186. There is a 2.6% chance that there will be no beds available when a patient arrives.Case 5: Thirteen arrivals per day
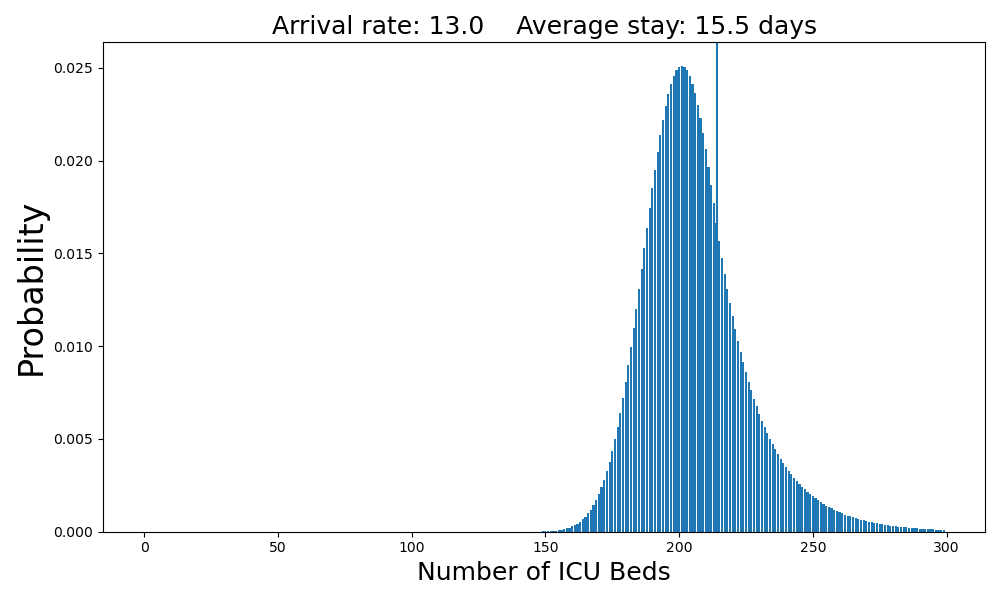
At thirteen arrivals per day, the system is overloaded.
The average number of occupied beds is 206. There is a 27% chance that there will be no beds available when a patient arrives.Case 6: 13.5 arrivals per day
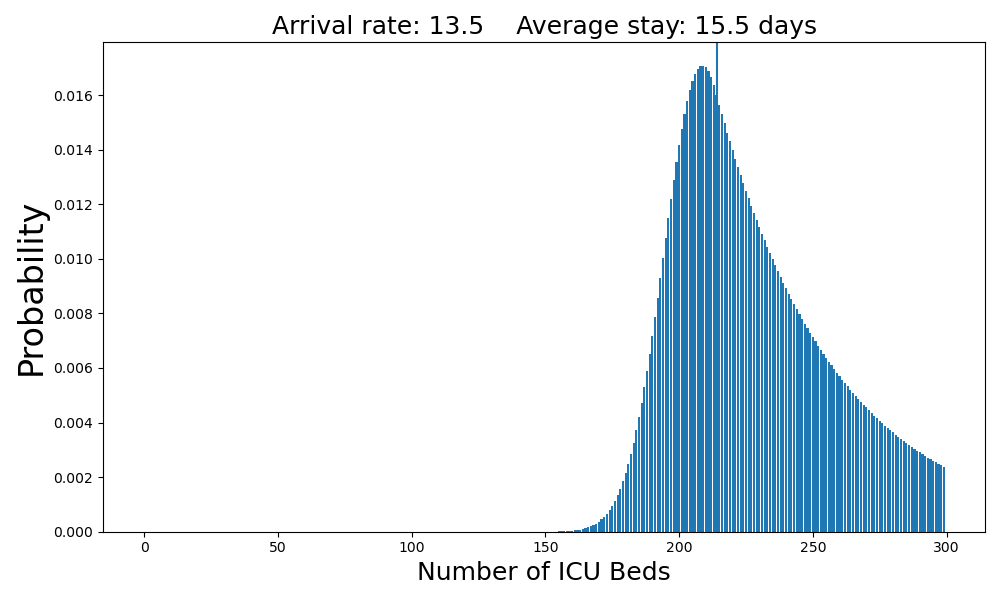
At 13.5 arrivals per day, the system is severely overloaded.
On average there are 13 patients waiting for beds. There is a 60% chance that there will be no beds available when a patient arrives.Case 7: 14 arrivals per day
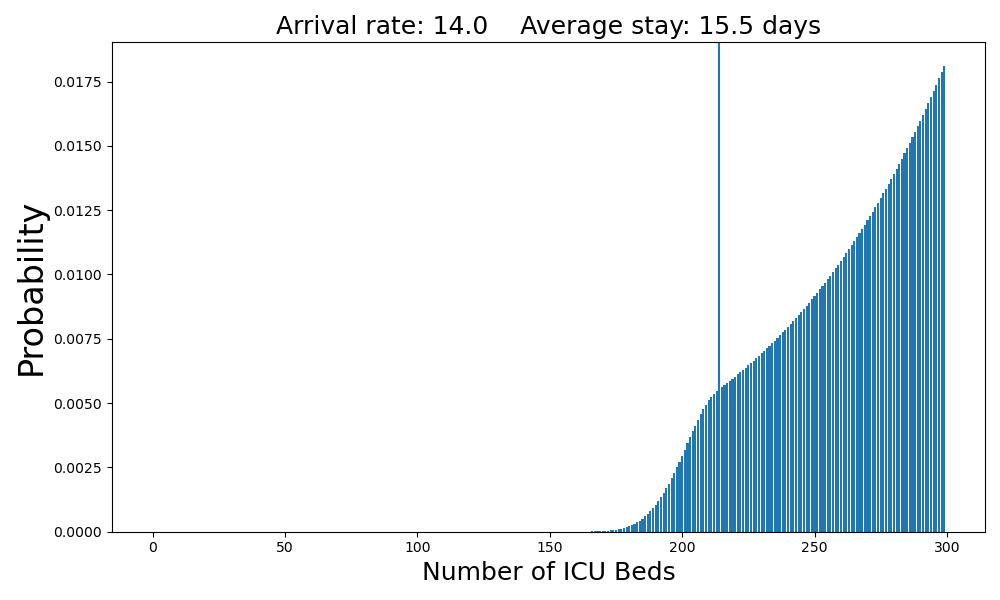
At 14 arrivals per day, the system has become unstable - there is no equilibrium. Arriving patients simply pile up in the queue.
My takeaway from this is that because of the long duration of ICU stays for severly ill SARS-CoV2-19 patients, it doesn't take that many cases per day to overwhelm the system.
My cousin Beth, a retired nurse, put it this way:5 "Ask parents to imagine they have a seven year old little girl who got hit by a car and they bring her to an overwhelmed emergency room, she lies on a stretcher in the hallway (not comfortable), you're standing next to her cries. You now know how much the unvaccinated have taken away your right for the care of your little girl. You will feel as helpless as the docs, nurses, and staff trying to keep up. We'll stay over into the next shift if needed, wearing PPE 12, 14, 16 hours a day." I'm vaccinated partly out of concern for my own health, and partly because I don't want to be one of the people taking up a place in the emergency room that a critically injured child might need.1MIT OpenCourseware Queueing theory course
2 A brief description of M/M/* models by Dr. Yih Huang of George Mason University (copyrighted material).
3ICU LENGTH OF STAY IN CRITICALLY ILL PATIENTS WITH COVID-19: DOES RACE MATTER? CHEST Journal Volume 160, ISSUE 4, SUPPLEMENT, A1164, October 1, 2021 .
4According to the Johns Hopkins Coronavirus website, Rhode Island has 214 beds in hospital Intensive Care Units.
5In the early 1980s Beth worked on one of the first dedicated AIDS wards in the country at Good Samaritan Hospital in West Islip, New York. At a time when no one knew how AIDS spread, some healthcare workers were afraid to enter a room with an HIV positive patient. Beth would go in; "Of course I'm going to go into that room. They're my patients". Today's healthcare workers are in a similar situation.
Computations were done with this Jupyter notebook